Perioperative management - Open tracheostomy - general and visceral surgery
You have full access to this content.
Indications
- Prolonged mechanical ventilation for more than 21 days.
- Airway obstruction, e.g., due to injury or tumor
- Compared with translaryngeal intubation, open tracheostomy offers these benefits: – avoids injury to the arytenoid cartilages
– avoids mucosal lesions at the vocal cords and trachea as well as in mouth and nose
– reduces airway resistance (decreases the work of breathing)
– decreases dead space
– better securing option
– easier oral hygiene
– less analgesics and sedatives needed
– more convenient for patient (can speak and ingest oral diet, no foreign-body feeling)
– enables or facilitates weaning
Contraindications
- Infection at the planned incision site
- Unstable cervical spine
- Coagulation disorders
- Massive gas exchange disorders
Preoperative diagnostic work-up
- Coagulation panel
- Bronchoscopy
Special preparation
None
Informed consent
- Bleeding
- Infection
- Tracheal injury
- Possible necessity of revision surgery
- Pneumothorax
- Injury to the recurrent nerve
- Cutaneous/mediastinal emphysema
- Scar formation at the tracheostomy
- Cardiac arrest by vagal stimulation
Anesthesia
- General anesthesia of less than 45 minutes
- Standard monitoring of vital parameters (ECG, NIBP, NMT, partial pressure of oxygen)
- Anesthesia induced with propofol, remifentanil and mivacurium
- Anesthesia maintained with propofol and sufentanil
Positioning
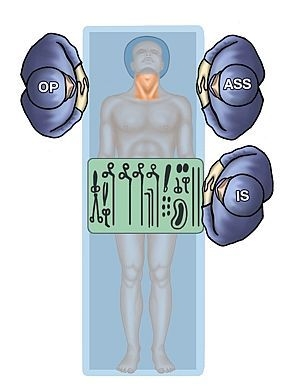
Operating room setup
Special instruments and fixation systems
- Complete sterile tracheostomy kit with drapes, OR gowns and sterile gloves
- Appropriately sized tracheostomy tubes for adults with an outside diameter of 9-12 mm and the largest lumen possible with 8.5-9.5 mm
- Guide rod
- Sutures
- Suction unit with catheter
- Materials for anesthesia, OR light, ECG monitor
- Skin prepping solution
- Electrosurgery unit
- Sterile dressing material
Postoperative management
- Airway hygiene: In order to keep the airways clear and prevent infections and atelectasis in patients on mechanical ventilation, the bronchial secretions must be suctioned.
- The dressing around the tracheostomy should be changed at least once daily, more often in case of marked secretion. To prevent wound infections, the dressings must always be changed under sterile conditions.
- Humidifying the inspired air: Since the tracheostomy bypasses the upper airways, their functions must be replaced by artificial means. Primarily this includes warming and humidifying the inspired air.
- Cuff pressure monitoring: During mechanical ventilation, the cuff ensures that inspired gas cannot escape from the trachea or liquid enter it. In order to prevent any tracheal injuries, only tubes with low-pressure cuffs are used in prolonged mechanical ventilation. Cuff pressure can be monitored with dedicated pressure gauges and should be about 10-20 mmHg.
Leave the tracheostomy tube in place for the first 48 hours after surgery because a permanent canal will not have formed yet. Later, cannula changes are once weekly in most cases.