Perioperative management - Aortobifemoral bypass for peripheral arterial disease Fontaine stage IIb–III - vascular surgery
You have not purchased a license - paywall is active: to the product selection
Indications
Depending on the length of the local occlusion/stenosis, the TASC III criteria suggest the treatment options to be used. The length of the stenosis and the region where it is located determine the general type of management: Endovascular or open vascular surgery.
TASC II classification in aortoiliac occlusion
Lesion type Morphology Recommended treatment A
Short (<3 cm) unilateral or bilateral stenosis of the CIA or EIA Endovascular B
Single or multiple stenosis totaling 3–10 cm involving the EIA, not extending into the CFA; and/or unilateral CIA occlusion Endovascular C
Bilateral CIA occlusion;[MM3] bilateral EIA stenoses 3–10 cm long not extending into the CFA; unilateral complete EIA occlusion Open reconstruction D
Diffuse disease involving the aorta and both iliac arteries requiring treatment; unilateral occlusions of both CIA and EIA; bilateral occlusions of EIA Open reconstruction Video example
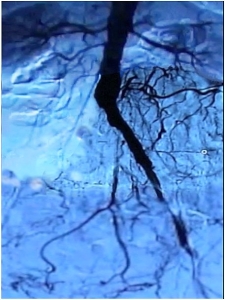
Clinically the patient is classified as Fontaine PAOD IIb–III and the preoperative angiogram demonstrates: Occlusion of the right CIA and EIA, subtotal stenosis of the left EIA and bilateral stenosis of the femoral bifurcation
-> TASC D, , thus recommendation for open revascularization
PAOD classification according to Fontaine and Rutherford
Fontaine stage
Clinical symptoms
Rutherford
Grade
Clinical symptoms
I
Asymptomatic 0
0
Asymptomatic IIa
Distance > 200 m 1
I
Mild claudication IIb
Distance< 200 m 2
I
Moderate claudication 3
I
Severe claudication III
Ischemic rest pain 4
II
Ischemic rest pain IV
Ulcers or gangrene 5
III
Ischemic ulceration not exceeding ulcer of the digits of the foot 6
III
Severe ischemic ulcers or frank gangrene Contraindications
- Serious cardiopulmonary risks (e.g., NYHA IV, COPD GOLD stage IV)
- Acute or chronic inflammatory abdominal disease (e.g., florid ulcerative colitis, recurrent sigmoid diverticulitis)
- History of multiple extensive abdominal procedures ("hostile abdomen")
- Cirrhosis
- Advanced malignancy
Preoperative diagnostic work-up
Medical history
- Claudication
- Distance walking without complaints
- Risk factors -> nicotine; arterial hypertension; CHD; heart failure; diabetes; manifest renal failure with/without dialysis; coagulation disorder
Inspection
- Skin changes
- Muscular abnormalities
- Orthopedic deformities
- Skin color
- Hair
- Trophic changes
- Swelling; edema; mycosis; phlegmon; leg ulcers etc.
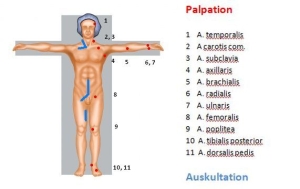
Palpation with contralateral comparison
- Arterial pulse examination
- Skin temperature
Arterial auscultation of the extremities with contralateral comparison
Ankle-Brachial Index (ABI)
- ABI = systolic BP of posterior tibial artery / systolic BP of brachial artery
ABI Severity of PAOD > 1.3 false high values (suspected Mönckeberg arteriosclerosis, e.g. in diabetes) > 0.9 Normal finding 0.75 - 0.9 Mild PAOD 0.5 - 0.75 Moderate PAOD < 0.5 Severe PAOD - An ABI of < 0.9 demonstrates the presence of significant PAOD.
- Noninvasive Doppler ultrasound measurement of the Ankle-Brachial Index (ABI) is an adequate test for the presence of PAOD.
- For the diagnosis of PAOD, the ABI with the lowest posterior tibial artery pressure is used.
- A pathologic ankle-arm index is an independent risk indicator for increased cardiovascular morbidity and mortality.
Color coded duplex sonography
- Carotid arteries, abdominal aorta, arteries of the extremities
- Localization of stenoses and occlusions in almost all vascular regions except the chest
- Quantifies the degree of stenosis and allows assessment of plaque morphology
- Sensitivity and specificity about 90%.
- Well suited for screening purposes
CT angiography
- Multi-slice computed tomography (MS-CT) with non-ionic contrast medium
- Broad range of indications: Traumatic vascular lesion (especially trunk); vascular dissection/rupture; aneurysm; arterial thrombosis/embolism; portal vein/mesenteric vein thrombosis; pulmonary artery embolism; PAOD; vascular tumors
- Pros: Fast; detection of significant concomitant disease; imaging of peripheral arteries; sensitivity and specificity each about 90%.
- Cons: Exposure to radiation and contrast media, allergies ( about 3%), no functional assessment
Cardiac check-up
- Resting ECG
- Exercise ECG
- Echocardiography
Chest radiograph
Possibly spirometry
Clinical chemistry
- RBC
- Electrolytes
- Coagulation
- Renal function
- Liver function
- Blood lipids
- Blood group
Special preparation
- Enema evening before surgery
- Hair trimmed in surgical field
- Packed RBCs ordered
- Foley catheter
- Perioperative prophylactic antibiotics 30 minutes before surgery (see German KRINKO and Robert-Koch-Institut recommendations)
Informed consent
General surgical risks
- Major bleeding; blood transfusions; hepatitis/HIV transmission from allogeneic blood units.
- Allergy/incompatibility
- Wound infection
- Thrombosis/embolism
- Injury to skin, vessels, nerves, e.g. due to positioning.
- Keloids
- Incisional hernia
Specific surgical risks
- Thrombosis of grafts and possibly regions supplied by runoff vessels, possibly leg ischemia, amputation
- Graft infection with suture bleeding; sepsis; leg ischemia; amputation
- Injury to adjacent organs such as ureter, bladder, spleen, liver; intestinal ischemia -> resection, colo-/ileostomy
- Paraplegia in artery of Adamkiewicz with low origin
- Nerve lesions -> paresthesia; pain; paralysis of the abdominal wall and thigh muscles
- Peritoneal adhesions -> chronic pain, mechanical ileus
- Lymphatic fistula
- Secondary bleeding
- Impotence
- Anastomotic/graft aneurysm
- Impaired renal function by intraoperative angiography
Anesthesia
Positioning
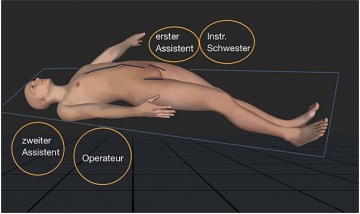
Operating room setup
Special instruments and fixation systems
Postoperative management
Single Access
Access to this lecture
for 3 days
€4.99 inclusive VAT

webop-Account Single
full access to all lectures
price per month
for the modul: General Surgery