Perioperative management - Aortoiliac TEA (thromboendarterectomy) in bilateral stage IIb peripheral arterial (occlusive) disease (PAD) - Vascular surgery - vascular surgery
You have not purchased a license - paywall is active: to the product selection
Indication
The TASC II criteria recommend therapeutic treatment options depending on the length of the local occlusion/stenosis. The length of the stenosis and its regional location determine the treatment: endovascular or open vascular surgery.
TASC II classification of aortoiliac lesions
Type
Morphology
Procedure
A
Unilateral or bilateral CIA stenosis; unilateral or bilateral short single (<3 cm) EIA stenosis
Endovascular
B
Single or multiple stenosis totaling 3–10 cm involving the EIAnot extending into the CFA and/or unilateral CIA occlusion
Endovascular
C
Bilateral CIA stenoses; bilateral EIA stenosis, 3–10 cm long, not extending into the CFA; unilateral EIA occlusion; bilaterasl CIA occlusions
Open revascularization
D
Diffuse disease involving the aorta and both iliac arteries requiring treatment; bilateral EIA occlusions; unilateral occlusions of both CIA and EIA; infrarenal aortoiliac occlusion; diffuse multiple stenosis involving the unilateral CIA, EIA and CFA
Open revascularization
Video example:
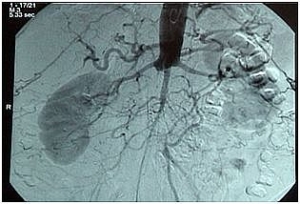
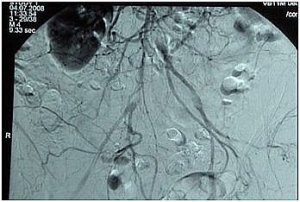
High aortic occlusion with subtotal stenosis of the iliac bifurcation, occlusion of the right CIA and thrombosis at the left EIA (bilateral clinical Fontaine stage IIb).
-> TASC II D, hence recommendation for open revascularization
Preoperative intra-arterial DSA
Classification of PAD according to Fontaine stage and Rutherford category
Fontaine stage
Presentation
Rutherford category
Grade
Presentation
I
Asymptomatic
0
0
Asymptomatic
IIa
Mild claudication (> 200 m)
1
I
Mild claudication
IIb
Moderate to severe claudication (< 200 m)
2
I
Moderate claudication
3
I
Severe claudication
III
Ischemic rest pain
4
II
Ischemic rest pain
IV
Ulceration or gangrene
5
III
Minor tissue loss
6
III
Major tissue loss
Contraindication
- Serious cardiopulmonary risks (e.g. NYHA IV, COPD Gold stage IV)
- Acute or chronic inflammatory abdominal processes (e.g., florid ulcerative colitis, recurrent sigmoid diverticulitis)
- History of multiple extensive abdominal procedures (“hostile abdomen”)
- Liver cirrhosis
- Advanced malignancy
- Transmural calcification of the aorta and pelvic axis*
- Abdominal aortic aneurysm*
in such cases: Y-graft
Preoperative diagnostic work-up
Medical history
- Claudication
- Walking distance
- Risk factors -> nicotine abuse; arterial hypertension; coronary heart disease; cardiac failure; diabetes, manifest renal failure with/without dialysis; coagulopathy
Inspection
- Skin changes
- Muscular abnormalities
- Orthopedic malalignment
- Skin color
- Body hair
- Trophic changes
- Swelling, edema, mycosis, phlegmon, leg ulcers
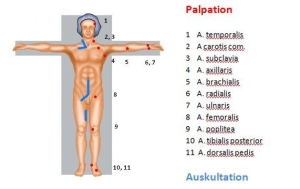
Palpatory bilateral comparison
- Pulse status
- Skin temperature
Auscultatory bilateral comparison of the limb arteries
Ankle-Brachial Index (ABI)
- ABI = systolic BP of posterior tibial artery / systolic BP of brachial artery
ABI value
PAD severity
> 1.3
Falsely high values (suspected Mönckeberg medial sclerosis, e.g. in diabetes)
> 0.9
Normal finding
0.75 - 0.9
Mild PAD
0.5 - 0.75
Moderate PAD
< 0.5
Severe PAD
- ABI < 0.9 is considered evidence of significant PAD.
- Determining the ankle-brachial index (ABI) through non-invasive Doppler occlusion pressure measurement is a suitable test for confirming PAD.
- PAD diagnosis is determined by the ABI value with the lowest ankle artery pressure.
- A pathologic ankle-brachial index is an independent risk indicator for increased cardiovascular morbidity and mortality.
Color flow Doppler ultrasonography
- Carotid arteries, abdominal aorta, limb arteries
- Stenoses and occlusions in almost all vascular regions apart from chest
- Allows quantifying the degree of stenosis and assessing plaque morphology
- Sensitivity and specificity around 90%
- Well suited as screening modality
CT angiography
- Multislice computed tomography (MS-CT) with nonionic contrast agent
- Broad range of indications: traumatic vascular lesion (esp. trunk); vascular dissection/rupture; aneurysm; arterial thrombosis/embolism; portal vein/mesenteric vein thrombosis; pulmonary artery embolism; PAD; vascular tumors
- Benefits: rapid; detects relevant comorbidities; visualizes peripheral arteries; sensitivity and specificity each about 90%.
- Drawbacks: Radiation and contrast agent exposure, allergies (about 3%), no functional assessment.
Angiography (intra-arterial DSA)
- Most often performed as digital subtraction angiography (DSA)
- Contraindication: hyperthyroidism; manifest renal disease; creatinine elevation relative to indication; metformin-containing antidiabetics (risk of lactic acidosis); PT < 30%.
- Benefits: visualization in highest detail; superselective imaging possible; immediate intervention possible; sensitivity 100%, specificity 100%.
- Drawbacks: Radiation exposure; contrast medium exposure; only patent vessels can be visualized while thrombosed regions and extravascular processes remain hidden; puncture and catheter complications.
- TSH and creatinine levels must be determined prior to DSA
- Caution in patients with multiple myeloma -> renal failure
Cardiac check
- Resting ECG
- Exercise ECG
- Echocardiography
Chest x-ray
Possibly spirometry
Laboratory panels
- Blood count
- Electrolytes
- Coagulation
- Kidney function parameters
- Liver function parameters
- Blood lipids
- Blood group
Special preparation
- Enema the evening before
- Hair cut in surgical field
- Order packed RBCs
- Foley catheter
- Administer prophylactic perioperative antibiotics 30 min. before beginning surgery (see KRINKO recommendation, Robert Koch Institute)
- Enema the evening before
- Hair cut in surgical field
- Order packed RBCs
- Foley catheter
- Administer prophylactic perioperative antibiotics 30 min. before beginning surgery (see KRINKO recommendation, Robert Koch Institute)
Informed consent
General surgical risks
- Major bleeding, blood transfusions, transmission of hepatitis/HIV through allogeneic blood transfusions
- Allergy/intolerance
- Wound infection
- Thrombosis/embolism
- Skin/vascular/nerve damage, e.g. due to patient positioning
- Keloid
- Incisional hernia
Specific procedural risks
- Thrombosis, possibly leg ischemia, amputation
- Infection with secondary suture bleeding; sepsis; leg ischemia; amputation
- Damage to adjacent organs, e.g., ureter; bladder; spleen; liver; intestinal ischemia -> resection, ostomy
- Paraplegia in the presence of deep origin of artery of Adamkiewicz
- Nerve lesions -> dysesthesia; pain; paralysis of abdominal wall / thigh muscles
- Peritoneal adhesions -> chronic pain, mechanical ileus
- Lymph fistula
- Secondary bleeding
- Impotence
- Deterioration of renal function induced by intraoperative angiography
Anesthesia
Positioning
Operating room setup
Special instruments and fixation systems
Postoperative management
Single Access
Access to this lecture
for 3 days
€4.99 inclusive VAT

webop-Account Single
full access to all lectures
price per month
for the modul: General Surgery