Perioperative management - Iliacomesenteric venous bypass in superior mesenteric artery occlusion—Vascular Surgery - vascular surgery
You have not purchased a license - paywall is active: to the product selection
Indications
- Intestinal angina due to short segmental stenosis of the superior mesenteric artery (SMA) close to its origin or occlusion due to inadequate collateral blood supply via the celiac trunk
- Lack of indication for interventional treatment, e.g., in long stenosis at the origin stenosis/occlusion of the SMA).
- Failure of interventional management
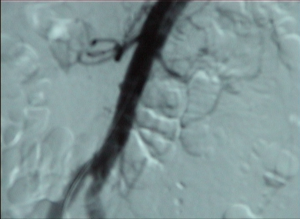
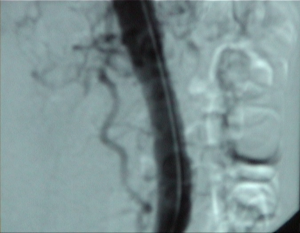
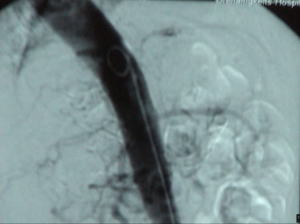
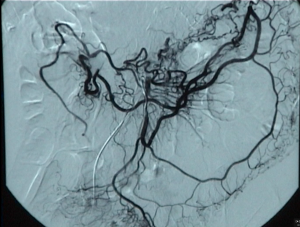
Video clip: SMA occlusion close to its origin with occlusion of the celiac trunk
Grade of ischemia and general indication for surgery
Stage Symptoms Indication for surgery I Asymptomatic Optional in concurrent procedures for vascular occlusion, aortic or iliac artery interventions II Intestinal angina = crampy postprandial abdominal pain, cachexia Absolute indication for surgery III Abdominal pain at rest Absolute indication for surgery IV Acute abdomen secondary to mesenteric infarction, intestinal gangrene, possibly peritonitis due to transmural bacterial translocation Emergent indication for surgery Contraindications
- long-distance and multifocal stenoses of the SMA > 6 cm usualy do not lend themselves to open repair
- Multisegment occlusive processes of the SMA, e.g. in thrombangitis obliterans (Winiwarter-Buerger disease) or lupus erythematosus
- ASA IV
- COPD Cold IV
Preoperative diagnostic work-up
Key aspects first:
1. Chronic intestinal ischemia syndromes: Only diagnostic imaging yields useful insights!
2. Usually there are multiple (vascular) comorbidities -> detailed examination by vascular surgeons and angiologists.
3. Patient should undergo work-up to identify other abdominal diseases, especially to rule out malignancies.
4. Delayed diagnosis > 12 months because differential diagnosis included the disease too late.
Medical history
Typical triad in malperfusion of the SMA:
- postprandial abdominal pain starting shortly (about 20 min) after food intake and subsiding after 3-4 hours (intestinal angina)
- reactive restriction on food intake -> weight loss, muscle atrophy, asthenia ("small-meal-syndrome")
Absence of weight loss does not rule out the diagnosis!
Ischemia of the celiac trunk distribution site results in nausea, vomiting, and meteorism; constipation is more likely to result from inferior mesenteric artery disease.
Duplex ultrasonography for assessment of the intestinal vessels
- Stenosis typically at the origin
- Increased flow rate—flow rates greater than 200 cm/s are considered pathognomonic for high-grade stenosis—as well as turbulent flow
CT angiography or MR angiography
- with image reconstruction
digital subtraction angiography of the intestinal arteries in 2 planes
- when planning an intervention
Abdominal ultrasonography
(Exercise) ECG
Chest X-ray
Laboratory panels
- Blood count, electrolytes, coagulation, renal retention parameters, blood lipids
Staged diagnostic approach to intestinal ischemia
Stage I:
Stage II
Stage III
Stage IV
Medical history and clinical examination +
+
+
+
Duplex ultrasonography +
+
+
Ø
angiography Ø
+
+
+
CT/MR angiography Ø
+
+
Ø
Special preparation
- Ultrasound assessment of whether an autologous great saphenous vein is available as a bypass (possibly synthetic graft)
- Identify blood group, provide for packed RBCs, if needed
- Enema
- Indwelling urinary catheter
Informed consent
General surgical risks
- Major bleeding, blood transfusions, transmission of hepatitis/HIV through allogeneic blood transfusions
- Allergy/intolerance
- Wound infection
- Thrombosis/embolism
- Skin/vascular/nerve damage, e.g., due to patient positioning
- Keloid
Risks special to this procedure
- Incisional hernia
- Abdominal adhesions, ileus
- intraoperative peripheral embolism in iliac/leg arteries -> surgical intervention, in case of ischemic leg including amputation
- Massive infection → bleeding, peritonitis, sepsis; possible reoperation with explantation of the vascular graft
- Injury to neighboring organs (ureter, bladder, bowel, liver, spleen); intestinal stoma
- Impaired perfusion or nerve injury of the spinal cord (paresis, erectile dysfunction)
- In case of autologous vein bypass: Secondary bleeding, infection, keloid
- Intraoperative angiography: Contrast agent → renal failure
- Bypass infection/stenosis → impaired perfusion of the affected organs, reoperation
- Impaired intestinal perfusion → defecation disorder, malabsorption, ischemic colitis → resection, possibly colostomy
Anesthesia
Positioning
Operating room setup
Special instruments and fixation systems
Postoperative management
Single Access
Access to this lecture
for 3 days
€4.99 inclusive VAT

webop-Account Single
full access to all lectures
price per month
for the modul: General Surgery