Perioperative management - Popliteal artery aneurysm: Resection and revascularization with greater saphenous vein graft (posterior access) - vascular surgery
You have not purchased a license - paywall is active: to the product selection
Indications
Management of popliteal artery aneurysms (PAA) aims to prevent major amputations caused by microemboli in the arteries of the lower leg from the aneurysm. In critical ischemia caused by PAA the rate of major amputation is between 25% and 50%.
Asymptomatic PAA
Surgery is generally recommended for aneurysms measuring 2 cm in diameter and more, since even small aneurysms often become symptomatic. Since in aneurysms smaller than 2 cm with partial wall thrombosis and no pedal pulses "silent" embolization may be possible, the indication for surgery this situation must be determined on a case-by-case basis.
Symptomatic PAA
Acute and chronic critical ischemia, local pressure consequences, venous thrombosis due to compression, septic aneurysm and rupture constitute an indication for surgery regardless of the length or diameter.
Contraindications
In thrombotic PAA occlusion with good collateralization and no intermittent claudication surgery is not mandatory. The indication for surgery in these cases depends on the perfusion situation of the extremity (e.g., PAOD stage III/IV). Autogenous distal crural bypass may be indicated. If the health of the patient is poor or the patient is unable to walk anymore, amputation may be an alternative.
Preoperative diagnostic work-up
History/Symptoms
At the time of diagnosis, 80% of PAA are clinically silent and about 14% become symptomatic each year. The symptoms resemble those in peripheral arterial occlusive disease:
- Arterial stenoses
- Microemboli
- Intermittent claudication
- Rest pain
- Trophic disorders
PAA may also manifest as swelling and secondary deep vein thrombosis of the leg.
Contralateral pulse status comparison
Occlusion pressure/ankle-brachial index
Color coded duplex sonography
Modality of choice:
- PAA screening and sizing
- Extent of mural thrombosis
- Runoff situation
- Anatomical variants
- also: preoperative mapping of the greater saphenous vein (= graft material)
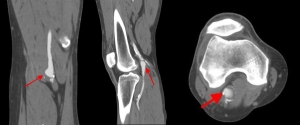
CT angiography
- complements ultrasonography for planning the surgical management of the PAA
Cardiac workup
- In suspected myocardial ischemia
Clinical chemistry
- RBC, electrolytes, coagulation panel
Chest radiograph
Screening for
- Aortic aneurysm (in about 20% of patients)
- Contralateral PAA (in about 50% of patients)
- Stenoses of the supraaortic branches require treatment
Special preparation
- If necessary, temporary discontinuation of oral anticoagulants with transition to low molecular weight heparin
- Preoperative mapping of the greater saphenous vein (= graft material)
Informed consent
General risks of surgery
- Allergy/incompatibility
- Wound infection
- Thrombosis/embolism
- Skin/tissue/nerve damage
- Keloids
Specific surgical risks
- Bleeding/secondary bleeding
- Hepatitis/HIV transmission by blood transfusion
- Arterial/venous thrombosis/embolism, microembolization
- Nerve damage
- Occlusion of the graft/bypass with critical ischemia, loss of extremities
- Massive infection of the graft/bypass
- Lymph edema/fistula of the leg
- Compartment syndrome
Anesthesia
Positioning
Operating room setup
Special instruments and fixation systems
Postoperative management
Single Access
Access to this lecture
for 3 days
€4.99 inclusive VAT

webop-Account Single
full access to all lectures
price per month
for the modul: General Surgery