Standard bilioenteric anastomosis - general and visceral surgery
You have not purchased a license - paywall is active: to the product selection
Principle
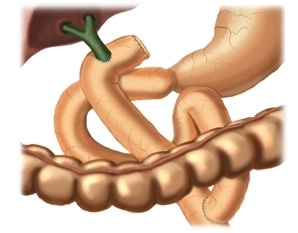
The gold standard in bilioenteric anastomosis is retrocolic end-to-side Roux-en-Y hepaticojejunostomy with a segment of the proximal jejunum.
Here, the preferred bilioenteric anastomosis is established proximal to the cystic duct and about 2-3 cm distal to the union of the hepatic ducts.
- The opening of the anastomosis should be as wide as possible (if the common hepatic duct is too small it may be enlarged with the Hepp-Couinaud technique)
- The single row of interrupted suture encompassing all layers should be leak-roof from the beginning and
- precisely adapt the mucosa of the hepatic duct to that of the jejunum.
Exploration – exposure of the hepatoduodenal ligament
The anastomosis will be explained as part of the Whipple procedure for cancer of the pancreatic head. One modification of the bilioenteric anastomosis (hilar hepatojejunostomy) is found under Hepp-Couinaud technique for bilioenteric anastomosis,
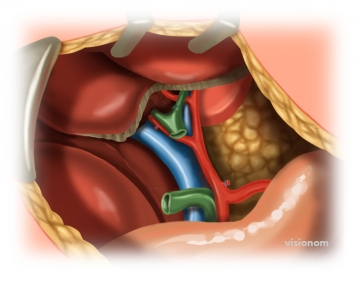
In the hepatoduodenal ligament expose the proper hepatic artery, portal vein and the CHD / CBD. Free the entire circumference of the duct.
Exposing the CBD/CHD
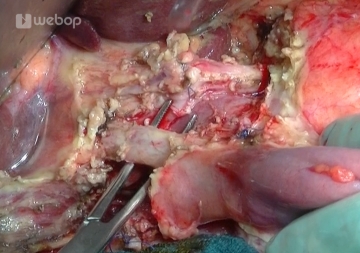
Once the circumference of the duct has been freed completely, it is divided immediately proximal to the junction of the cystic duct. The duodenal end of the CBD is closed with an absorbable running suture (Vicryl® 3-0) (not shown). The part to be anastomosed is temporarily blocked with bulldog forceps.
Note: Because of the clinically significant preoperative obstruction of the CBD, it had been decompressed before surgery by a blue drain through a stent.
Dissecting the jejunal loop
A detailed description of the Roux-en-Y technique is found here Gastrointestinal anastomosis, Roux-en-Y esophagojejunostomy
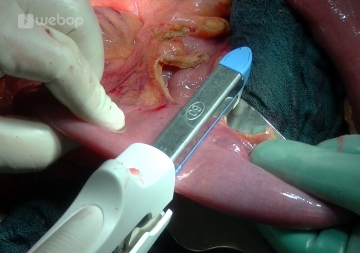
Free the 2nd jejunal loop. Identify the mesenteric vascular arcades by transillumination and dissect with the Ligasure. Divide the loop at a location with confirmed blood flow. Pull up the descending Roux-en-limb through a window in the mesentery to the right of the middle colic artery. Verify that the mesentery is not twisted. Stitch over the stapled blind end with a running seromuscular suture PDS 5/0.
Creating the bilioenteric anastomosis – suturing the posterior wall
Creating the bilioenteric anastomosis – suturing the anterior wall
Closing the mesenteric window
Single Access
Access to this lecture
for 3 days
€4.99 inclusive VAT

webop-Account Single
full access to all lectures
price per month
for the modul: vascular surgery