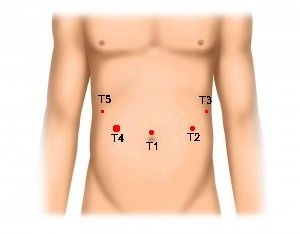
Start the procedure by marking the trocar positions on the abdominal wall. After inserting the Veress needle and pressure-controlled CO2 insufflation, place the following trocars in a semicircle:
- T1 = camera trocar (10 mm)
- T2 = working trocar(10 mm)
- T3 = working trocar 5 mm (later 12 mm for CEEA stapler and extension of incision for specimen retrieval)
- T4 = working trocar (12 mm)
- T5 = working trocar (5 mm)