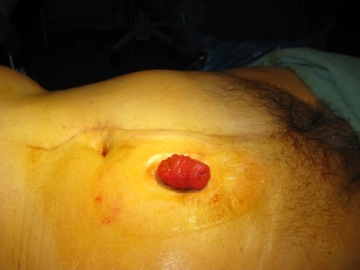
Usually (in about 70% of cases), the issue of ileostomy construction arises in the treatment of underlying abdominal malignancy (colon, rectum, bladder) either to stave off possible ileus in neoadjuvant or palliative radiochemotherapy and/or to prevent postoperative complications (anastomotic stenosis or failure).
Also in:
- Crohn disease, ulcerative colitis
- Familial adenomatous polyposis (FAP)
- Malformations
- Intestinal ischemia
- Protective ileostomy in major intestinal operations
- Protective ileostomy before, e.g., extensive proctological procedures (fistula surgery)
- Anastomotic failure
- Palliation in inoperable underlying disease with impending ileus