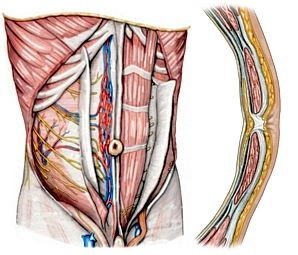
Superficial layer
The superficial layer of the abdominal wall comprises the skin and the fatty tissue underneath (panniculus adiposus telae subcutaneae abdominis).
Middle layer
The middle layer primarily comprises the anterior and posterior abdominal muscles with their fascias.
Anterior abdominal muscles and rectus sheath
The anterior abdominal muscles comprise three rather flat muscles and the rectus abdominis. Anteromedially the flat muscles fuse with the rectus sheath and insert there with a broad tendon (aponeurosis). The muscles course in the following anteroposterior order:
- External oblique: Posteriorly, it originates at the thoracolumbar fascia and the inferior 7 ribs and then courses as anterior lamina of the rectus sheath to the median linea alba and the iliac crest of the pelvis. Its oblique fibers run superolaterally to inferomedially.
- Internal oblique: It courses from the linea alba to the iliac crest and the anterior margin of the pubic bone. Its oblique fibers run superomedially to inferolaterally (continuing the contralateral external oblique). Thus, both muscles crisscross obliquely in the anterior abdominal wall. Superior to the arcuate line, the internal oblique fuses with both the anterior and posterior lamina of the rectus sheath, and inferior to the arcuate line only with the anterior lamina.
- Transversus abdominis: Its fibers course anteriorly from the thoracolumbar fascia or the cartilage of the inferior ribs and the pelvis to the linea alba. In the superior region of the anterior abdominal wall it primarily constitutes the posterior lamina of the rectus sheath. Together with the oblique abdominal muscles it constitutes the anterior lamina inferior to the arcuate line. The transversalis fascia constitutes the posterior wall of these three muscles.
- On both sides the rectus abdominis originates at the cartilage of ribs 5-7 and inserts in the pubic bone near the symphysis pubis. Tendinous intersections divide the long muscles into several bellies (“six-pack”). The pyramidalis muscle is an inconsistent muscle coursing anterior to the rectus abdominis and bracing the linea alba. Thus, the rectus sheath is a tendinous canal investing the flat abdominal muscles and comprising the rectus abdominis and pyramidalis muscle as well as various vessels and nerves (inferior and superior epigastric artery and vein, intercostal nerves 5-12).
Function
For flexion and rotation of the trunk and abdominal straining both oblique abdominal muscles (m. obliquus externus and internus abdominis - oblique cross) and the rectus abdominis plus transversus abdominis (upright cross) brace the anterior abdominal wall in the fashion just described.
The cremaster muscle derives from the internal oblique and transversus abdominis. It is the muscular investment of the spermatic cord and can lift the testicles (cremasteric reflex).
Deep layer
The transversalis fascia is the deep posterior layer of the abdominal wall. As the most internal layer of connective tissue (only separated from the free abdominal cavity by the peritoneum), it covers the internal aspect of the rectus abdominis and transversus abdominis and conjoins with the arcuate line and inguinal ligament. The deep inguinal ring with the entry to the inguinal canal is situated inferolaterally.
Posterior muscles
The major posterior muscle of the abdominal wall is the quadratus lumborum, which courses below the transversus abdominis from the lowermost rib and costal processes of the lumbar spine to the iliac crest.
Blood supply and innervation
The arterial blood supply follows the above layers of the abdominal wall:
- The superficial and middle layers are supplied by the
- → inferior posterior intercostal arteries (including the subcostal artery),
- → superficial epigastric artery,
- → superficial circumflex iliac artery and the
- → external pudendal artery.
- The deep layer is supplied by the
- → lumbar arteries,
- → inferior epigastric artery,
- → deep circumflex iliac artery and the
- → iliolumbar artery.
The venous blood of the abdominal wall drains via veins (primarily → inferior vena cava) eponymic with their corresponding arteries:
Via the superficial epigastric vein (→ great saphenous vein) and the inferior epigastric vein (→ external iliac vein). The venous blood only enters the superior vena cava via the thoracoepigastric veins and the azygos and hemiazygos veins.
The abdominal wall is innervated by intercostal nerves and branches of the lumbar plexus:
- As noted above, the inferior intercostals (including the subcostal nerve) innervate the external oblique abdominal muscle and the rectus abdominis.
- The iliohypogastric nerve, originating at the lumbar plexus, innervates all anterior abdominal muscles, as does the ilioinguinal nerve except for the rectus abdominis, while the genitofemoral nerve supplies the transversus abdominis.
- The iliohypogastric and ilioinguinal nerves also course between the muscles innervated by them and supply the skin of the anterior abdominal wall.
Superior to the umbilicus, lymph from the anterior abdominal wall drains cephalad (into the axillary and parasternal lymph nodes), while inferior to the umbilicus it drains caudad (into the inguinal and iliac lymph nodes). Lymph from the lateral abdominal wall drains into the lumbar lymph nodes.