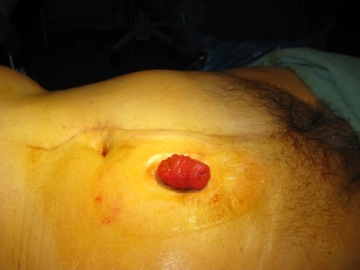
Stomas are often created during abdominal surgeries, whether in emergency situations or elective procedures.
The indication for and type of stoma creation depend on the underlying disease and the general situation.
- Neoplastic diseases → Prevention of ileus during neoadjuvant treatment or inoperability
- To protect high-risk anastomoses (protective ileostomy) or due to the removal of sphincters after radical oncological bowel resections
- Anastomotic insufficiency
- Emergency situations such as after abdominal trauma, intestinal ischemia, ileus, or bowel perforation
- Protective placement before, for example, extensive proctological procedures (fistula surgery)
- Chronic inflammatory bowel diseases
- Functional disorders such as severe fecal incontinence, evacuation disorder
- Congenital intestinal anomalies (malformations)
In the presented example, it is an ileostomy created during an open rectal carcinoma operation.
Types of stomas:
- Temporary versus permanent stomas, possibly considering the need for complete diversion of stool passage to keep the subsequent bowel segment dry.
- End stomas (split stomas, where the bowel ends after resection are separately diverted as end stomas) versus loop stomas (resection stomas where the bowel ends after resection are sutured posteriorly and then diverted together).
- Modified split stoma where the efferent limb of a loop stoma is blindly closed at the abdominal wall level. This combines the advantages of complete diversion of stool passage with those of easy reversal without re-laparoscopy or -tomy.
- Hartmann's situation with rectal blind closure and end colostomy. Here, a re-laparoscopy or -tomy is required in any case (reconnection surgery Hartmann II).
An end stoma is usually created when, at least in the long term, reversal is not planned or possible.
If the stoma is to be temporary, a loop stoma is usually created. A small bowel stoma is typically created in the terminal ileum or, if that is not possible, in the most distal small bowel segment.
Optimal is the transrectal placement in the lower abdomen above the arcuate line. The better muscular and fascial support here is intended to prevent a parastomal hernia or prolapse.
Due to anatomical proximity, the transverse stoma is best placed in the upper abdomen, and the ileo- and sigmoidostomy in the lower abdomen.
Special situation protective stoma in colorectal carcinoma:
In low anterior resection with TME, a protective stoma is generally indicated, with an ileostomy being preferable to a colostomy. An ileostomy is easier and less complicated to reverse. Parastomal hernias and stoma prolapses occur less frequently. However, fluid loss syndrome is much less common with a colostomy, and obstruction issues after reversal are also less frequent.