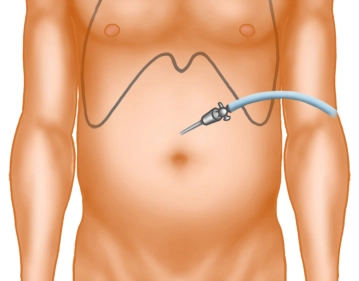
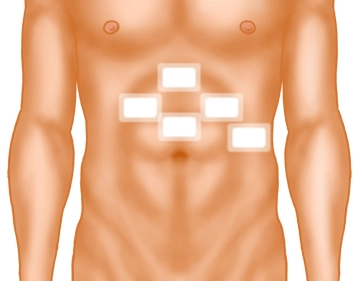
A small skin incision is made well above the navel in the midline. After inserting the Veress needle and verifying the correct position, the pneumoperitoneum is established.
-
Skin incision
-
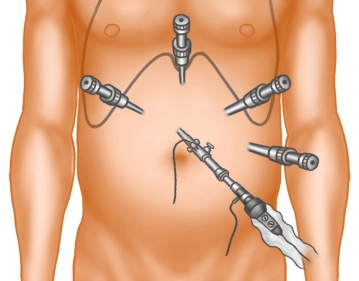
Trocar positioning
-
Traction of the stomach and incision of the lesser omentum
-
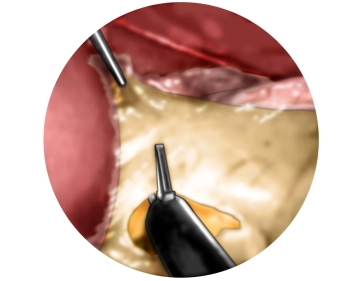
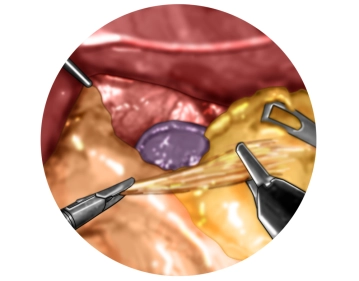
Preparation of the diaphragmatic crura with entry into the mediastinum
-
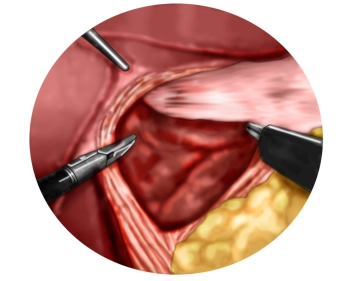
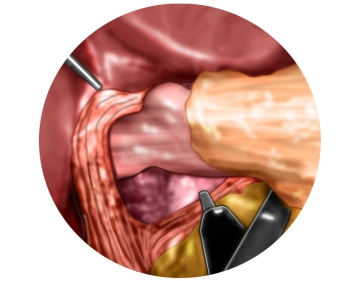
Preparation of the lower esophagus
![Preparation of the lower esophagus]()
Soundsettings One now proceeds far into the lower mediastinum and circumferentially mobilizes the lower esophagus from its adhesions. In doing so, the posterior vagus nerve is clearly identified and remains with the esophageal musculature. The esophagus is mobilized from the mediastinum to the extent that the area of the lower esophageal sphincter is tension-free in the abdominal cavity.
-
Mobilization of the gastric fundus
-
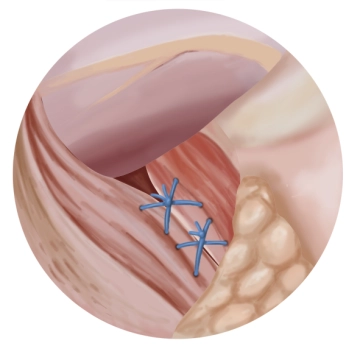
Posterior hiatoplasty
![Posterior hiatoplasty]()
Soundsettings A posterior hiatoplasty is performed using two Z-sutures (braided, non-absorbable suture size 1). The passage for the esophagus must remain sufficiently wide and well patent.
Tip: To avoid constriction of the terminal esophagus by the hiatoplasty, it is recommended to introduce a gastric tube Charrière (Ch) 40 as a calibration bougie transorally.
-
Shoeshinetest
-
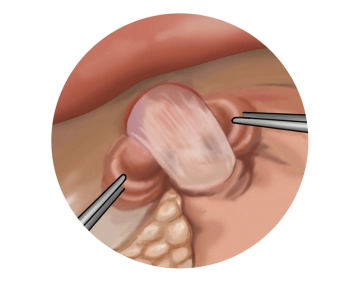
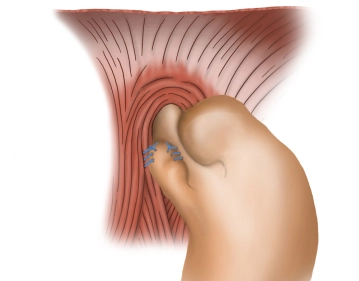
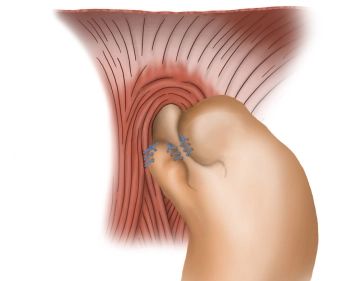
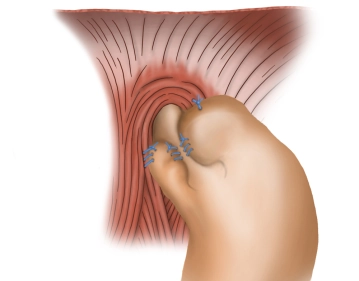
Fixation of the fundus cuff I
![Fixation of the fundus cuff I]()
Soundsettings The anterior vagus branch is clearly identified. While preserving it, the right fundus flap is initially continuously sutured to the right side of the esophagus (braided, non-absorbable suture size 2-0). Additionally, the fixation of the fundus portion pulled to the right is then performed with another continuous suture (braided, non-absorbable suture size 2-0) to the right diaphragmatic crus.
-
Fixation of the fundus cuff II
-
Fixation linker fundus
-
Suture and Dressing