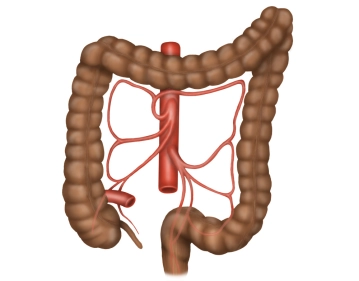
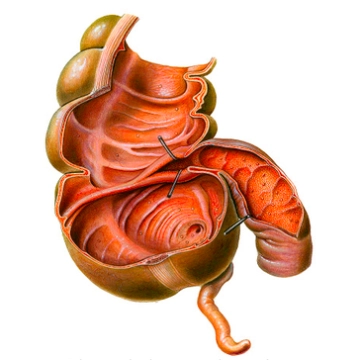
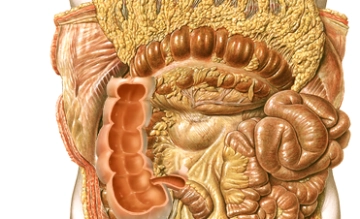
The colon frames the loops of the small intestine along the inner abdominal wall and below the liver and stomach. Its position is intraperitoneal or secondary retroperitoneal. The primary function of the colon is to thicken the chyme by absorbing water. The total length of the colon averages 120–150 cm. It begins at the ileocecal valve and ends at the rectosigmoid junction, transitioning into the rectum.
The colon is divided into the following sections:
- Cecum (or Caecum) with the appendix
- Ascending colon
- Transverse colon
- Descending colon
- Sigmoid colon