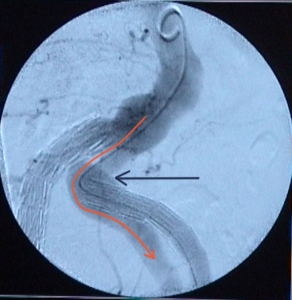
Perioperative management - Interventional management of type Ia endoleak after endoluminal repair of bilateral internal iliac artery aneurysms - Vascular Surgery - vascular surgery
You have not purchased a license - paywall is active: to the product selection
Indications
Endoleak classification
Type I
Inadequate sealing of landing zones
- A: proximal fixation
- B: distal fixation
- C: iliac occluder in aortoiliac endograft and femorofemoral cross-over bypass
Type II
Retrograde blood flow in the aneurysm sac via collateral vessels (mainly nferior mesenteric artery and lumbar arteries, occasionally accessory renal artery)
- A: single vessel
- B: two vessels or more
Type III
- A: junctional separation of modular components
- B: Defect in graft fabric
Type IV
Generally porous graft (intentional design of graft, usually self-limiting)
Type V
Endotension (growing aneurysm without evidence of endoleak)
Type I and type III endoleaks are associated with a higher risk of aneurysm rupture-> prompt intervention recommended
Contraindications
- ASA IV
Preoperative diagnostic work-up
Thorough vascular surgery examination:
- Pulse status
- Doppler study of both legs
- Possibly walk test in case of concomitant PAOD and poor foot pulses on palpation
- Abdominal ultrasonography
- Carotid color doppler study
- Echocardiography
- Exercise ECG
- Laboratory panels (electroytes, coagulation, renal function, blood count, blood lipids)
- Chest X-ray
- Spiral CT -> exact dimensioning of the endografts required for the endoleak repair
Special preparation
- Identify blood group, provide for packed RBCs, if needed
- Remove the hair in the surgical field
- Possibly, place urinary catheter
- Prophylactic antibiotics are usually administered as recommended by the German Society for Vascular Surgery (single-shot cefuroxime 30 minutes before skin incision), but the benefit is currently subject to debate because of issues around antibiotic resistance (Robert-Koch-Institute).
Informed consent
General surgical risks
- Major bleeding, blood transfusions, transmission of hepatitis/HIV through allogeneic blood transfusions
- Allergy/intolerance
- Wound infection
- Thrombosis/embolism
- Skin/vascular/nerve damage, e.g., due to patient positioning
- Keloids (in open surgery)
Specific procedural risks
- Vascular injuries, e.g., during graft delivery: surgical hemostasis, blood transfusions, in case of massive bleeding or arterial rupture, immediate conversion to open surgery
- Pseudoaneurysm of the punctured vessels, arteriovenous fistula, seroma
- Inadequate graft fixation or leakage: corrective procedures, possibly open surgery
- Graft infection: possible after days, months, or even years; endocarditis, sepsis, leg ischemia, amputation; surgical removal of vascular graft
- Nerve lesions -> dysesthesia; pain; paralysis of abdominal wall / thigh muscles
- Lymph fistula
- Temporary or permanent lymphedema of the legs; compression stockings, lymphatic drainage
- Secondary bleeding
- Impotence
- Deterioration of renal function induced by intraoperative angiography, chronic dialysis
Risks due to impaired perfusion
- Thrombosis/embolism: pulmonary embolism, apoplexy, myocardial infarction; prophylaxis: heparin → HIT II risk
- Legs: thrombosis of the graft and possibly adjacent vascular segments, possibly leg ischemia, amputation (e.g., toes)
- Gluteal muscles: due to overstenting of the iliac arteries, in particular bilaterally; claudication during walking, possibly gluteal necrosis
Anesthesia
Positioning
Operating room setup
Special instruments and fixation systems
Postoperative management
Single Access
Access to this lecture
for 3 days
€4.99 inclusive VAT

webop-Account Single
full access to all lectures
price per month
for the modul: General Surgery