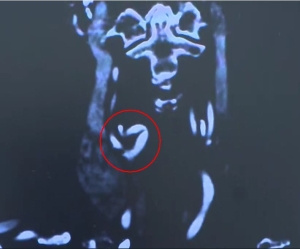
Perioperative management - Dolichoarteriopathy – Severe kinking with luminal narrowing type I/III of the right internal carotid artery - vascular surgery
You have not purchased a license - paywall is active: to the product selection
Indications
Surgical repair in carotid artery obstruction aims to prevent strokes and reduce the related disability and mortality rate.
Intervention is indicated in kinking with luminal narrowing of the internal carotid artery (ICA) in these conditions:
- neurological symptoms (TIA, amaurosis fugax, hemiparesis, stroke)
- high-grade bilateral kinking stenosis with a stenosis >70%, even without neurological symptoms
- Pseudo-occlusion due to kinking
Types of ICA kinking with luminal narrowing according to Weibel and Field*.
Type I
Tortuosity
Type II
Coiling
Type III
Kinking
*Weibel J, Fields WS (1965) Tortuosity, coiling, and kinking of the internal carotid artery.Neurology15, I 7±18, II 462±468.
Video example
Kontraindikationen
Nicht operationsbedürftig sind:
- asymptomatisches unilaterales Kinking mit mittelgradiger Stenose
- Coiling ohne Stenose als anatomische Variante
Preoperative diagnostic work-up
Medical history
- Vascular risk factors: Smoking, arterial hypertension, lipid metabolism disorders, diabetes
Clinical neurological examination
- > 90% of all stenoses and occlusions of supraaortic vessels (ICA, vertebral artery, etc.) remain clinically asymptomatic and are discovered as incidental findings in screening examinations or preoperative imaging
- The symptoms of a lesion in the vessels supplying the brain depend on the affected vessel, the course over time and the predominant collateralization (e.g. via the circle of Willis)
- Typical symptoms of a carotid artery (internal carotid artery) lesion include:
◊ motor or sensory hemi-symptoms (e.g. "hemiplegia/hemiparesis")
◊ Amaurosis fugax (temporary unilateral blindness: ophthalmic artery)
◊ cortical dysfunction (speech, visual-spatial perception)
◊ homonymous bilateral visual field restrictions are usually not characteristic symptoms of internal carotid artery stenosis
- Important: Carotid artery auscultation is not suited for detecting stenoses.
Cardiological examination
- 30% of patients present with CHD warranting treatment
Color-coded duplex sonography
Ultrasonography of the extracranial vessels supplying the brain should always examine all vessels in the transverse and longitudinal plane:
- Common carotid artery from proximally to carotid bifurcation
- Carotid bifurcation with dorsolateral internal carotid artery
- External carotid artery
- Vertebral artery in segments V1 to V3
- Subclavian and axillary arteries
Search for hemodynamically significant plaques and their morphological description (B-scan):
- Hyperechoic versus hypoechoic
- Homogeneous versus inhomogeneous
- Smoothly delineated versus irregular configuration
Plaque parameters with unfavorable prognosis:
- Hypoechoic internal plaque structure
- long plaque >1 cm
- Plaque diameter >4 mm
- Longitudinal pulsation of plaque distad
According to international agreement, stenoses should be quantified according to the NASCET criteria.
Contrast-enhanced MR angiography or alternatively a CT angiography
- Validation of the findings or for treatment planning
- Assessment of intracranial vessels and possible parenchymal damage (previous cerebral infarctions)
Digital subtraction angiography (DSA) of the arteries supplying the brain
- only if definite diagnosis is not possible with the noninvasive modalities and therapeutic consequences result
- Example: kinking with luminal narrowing not visible on MRT or CT
CT or MRI of the brain
- in symptomatic patients parenchymal imaging before planned revascularization
- in asymptomatic patients, such imaging can provide valuable additional information, e.g., evidence of clinically silent cerebral infarction
Chest radiograph
Clinical chemistry
- RBC
- Electrolytes
- Coagulation
- Renal function
- Liver function
- Blood lipids
- Blood group
In all patients with atherosclerotic carotid stenosis, look for any secondary sequelae of arteriosclerosis (coronary heart disease [CHD], peripheral arterial occlusive disease [PAOD])!
Special preparation
- Mark affected side
- Fasting for 2–6 hours, depending on clinical protocol.
- Continue platelet aggregation inhibitors; in DAPT decide each case according to the patient's cardiac risk profile
Informed consent
General surgical risks
- Major bleeding; blood transfusions; hepatitis/HIV transmission from allogeneic blood units.
- Allergy/incompatibility
- Wound infection
- Thrombosis/embolism
- Injury to skin, vessels, nerves, e.g. due to positioning.
- Keloids
Specific surgical risks
- Cerebral circulation problems/stroke
- Circulatory disorders of the eyes including blindness
- Injury to cervical nerves: Hoarseness; loss of voice; swallowing and breathing problems; facial paralysis; shoulder weakness
- secondary bleeding, hematoma-related tracheal compression, emergent surgical decompression
- Injury to glomus caroticum: Arrhythmias, fluctuating blood pressure
- Cardiopulmonary complications: Myocardial infarction, pneumonia, pulmonary embolism
- Hyperperfusion syndrome: Seizures; neurologic deficits; migraine headaches; cerebral edema and bleeding
- Suture aneurysm -> reoperation
- intraoperative angiography: contrast-induced acute kidney injury
Specific risks in surgery under regional anesthesia (cervical plexus block)
- Horner syndrome (drooping eyelid)
- Sensation of warmth in the face, hoarseness, breathing problems
- Concomitant anesthesia of adjacent structures: Brachial plexus, cervical spinal cord
Anesthesia
Positioning
Operating room setup
Special instruments and fixation systems
Postoperative management
Single Access
Access to this lecture
for 3 days
€4.99 inclusive VAT

webop-Account Single
full access to all lectures
price per month
for the modul: General Surgery