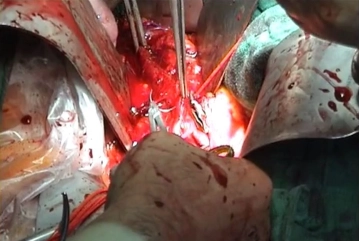
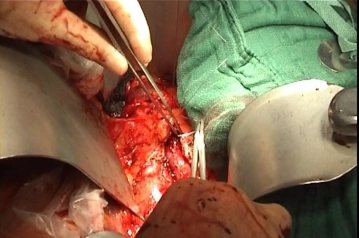
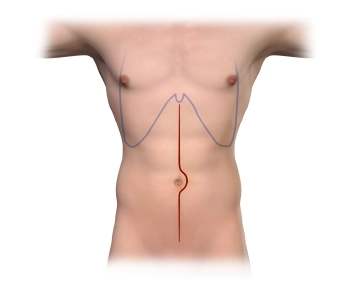
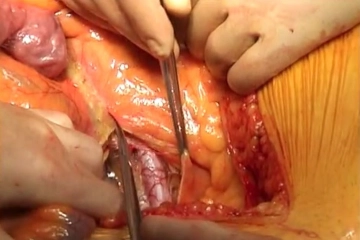
Close the aortotomy directly with a running suture (monofilament, 4/0 or 5/0 depending on the thickness of the aortic wall). Flush the aorta before finishing the suture and check for central run-in and peripheral run-off. After completing the suture, gradually release the blood flow under manual control of the compression. Counteract the heparin and remove all bulldog clamps still in place.
Tips:
1. Direct suturing of the aortotomy is biologically superior compared to synthetic patches, as in the long run patch plasty is prone to aneurysm formation, necessitating repeat procedures. However, direct suture of the aorta requires a diameter of at least 16 mm. Diameters of 14 mm and less, however, require patch plasty. This is also necessary once the arteriotomy is extended into the common iliac artery.
2. Check the bowel perfusion once the blood flow has been restored.
3. The color of the sigmoid at this stage of the procedure does not reveal anything about blood flow quality. If there is any doubt about the sigmoid blood flow, check the marginal arteries by Doppler ultrasonography.